
- English
- Español
- Português
- русский
- Français
- 日本語
- Deutsch
- tiếng Việt
- Italiano
- Nederlands
- ภาษาไทย
- Polski
- 한국어
- Svenska
- magyar
- Malay
- বাংলা ভাষার
- Dansk
- Suomi
- हिन्दी
- Pilipino
- Türkçe
- Gaeilge
- العربية
- Indonesia
- Norsk
- تمل
- český
- ελληνικά
- український
- Javanese
- فارسی
- தமிழ்
- తెలుగు
- नेपाली
- Burmese
- български
- ລາວ
- Latine
- Қазақша
- Euskal
- Azərbaycan
- Slovenský jazyk
- Македонски
- Lietuvos
- Eesti Keel
- Română
- Slovenski
- मराठी
- Srpski језик
Lumbar Puncture Needles: Evolution, Selection, and Clinical Practice
Lumbar puncture is a crucial clinical procedure, and the choice of instruments directly affects the therapeutic outcome and patient comfort. Lumbar puncture needles are mainly classified into three types: the traditional Quincke needle, the modern pencil-point needle, and the specialized combined spinal-epidural anesthesia needle, each with specific applications.
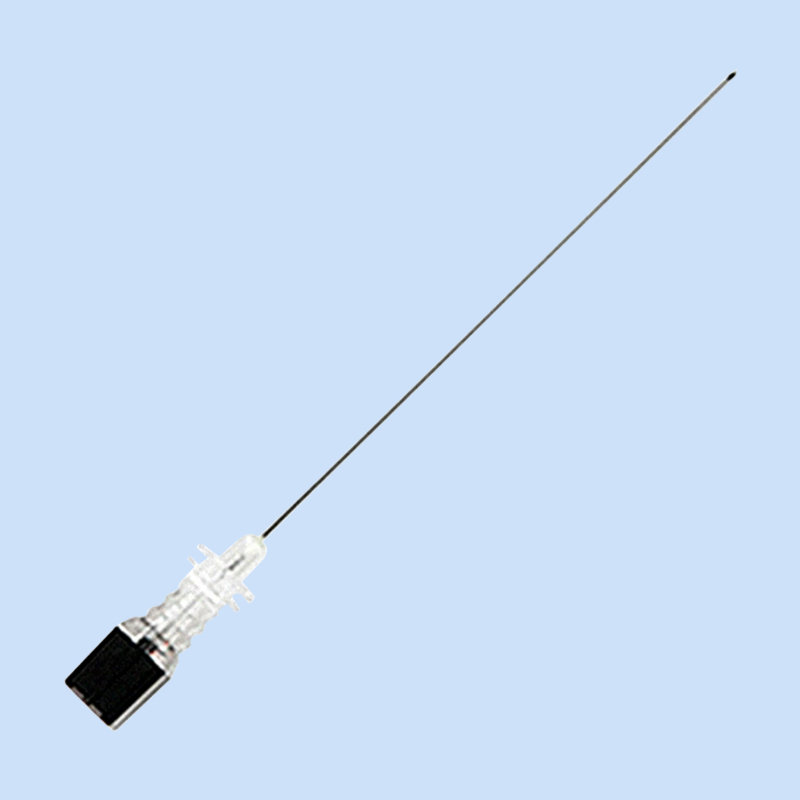
The Quincke needle features a beveled tip design, which makes it easy to penetrate the dura mater and provides a clear sense of operation. However, its cutting puncture leaves a relatively large opening in the dura mater, which is prone to causing cerebrospinal fluid leakage and increasing the risk of post-puncture headache.
The pencil-point needle features a conical blunt tip design. By pushing aside rather than cutting the fibers of the dura mater, it significantly reduces the incidence of cerebrospinal fluid leakage and headache. Although the sensation during puncture is less pronounced, its safety advantage makes it the preferred choice for most punctures.
The combined spinal-epidural anesthesia needle adopts an inner-needle design: first, the epidural needle is used for positioning, and then a thinner spinal anesthesia needle is inserted through its inner lumen. This design enables rapid spinal anesthesia and epidural catheter placement simultaneously, making it suitable for anesthesia that requires a long duration or precise control.

Overall, puncture needles are mainly used for diagnostic collection of cerebrospinal fluid and therapeutic injection of drugs or placement of catheters. In clinical selection, pencil-point needles are often chosen for diagnostic punctures to reduce complications, while dedicated needle sets are used for anesthesia needs. The evolution of puncture needles reflects the trend of clinical operations towards minimally invasive and patient-centered approaches, and the wide application of pencil-point needles is a manifestation of this concept.



